Recruitment information for muscle and cellular function study

We are seeking volunteers comprising 40 ME/CFS patients and 20 controls to participate in an NIH funded (U54AI178855) project. An overview of the study can be found here. Only those participants whose onset of ME/CFS was before 2020 will be eligible. Please review our recruitment flyer for more information on how to volunteer as a patient or control in this research study.
Large CPET publication describes the physiological component of post-exertional malaise in ME/CFS
Out in the Journal of Translational Medicine, Betsy Keller et al. describes results from the Center’s large multi-site 2-day CPET study. The publication analyzes cardiopulmonary exercise testing (CPET) data collected over two days from 84 individuals with ME/CFS and 71 sedentary controls. Within this population, 55 sex, age, and fitness-matched pairs were also compared. This is the largest 2-day CPET study of ME/CFS to date.
The article provides robust documentation of impaired recovery in people with ME/CFS following exertion (i.e., post-exertional malaise), something that is not seen in the control population. The study also recruited sedentary controls and used sex, age, and fitness-matched pairs to validate that fitness level does not predispose someone with ME/CFS to exertion intolerance. Keller et al. highlights that the autonomic nervous system is, at least partly, associated with ME/CFS due to the disrupted hemodynamic and ventilatory responses to exertion. Additionally, the worsening of CPET parameters over the two-day protocol led to increased clinical impairment status in ME/CFS whereas controls remain relatively the same.
Overall, the manuscript provides a detailed look at the physiological component of post-exertional malaise in ME/CFS. The paper is open access. Individuals interested in the topic should check out the full publication for more information.
Hanson presents at Demystifying Long COVID North American Conference 2024
Maureen Hanson spoke at the Demystifying Long COVID North American Conference, sponsored by Academic Medical Education organization, and her talk comparing ME/CFS with long COVID is now available online.
Center investigators present at International ME/CFS & Long COVID Conference
Center investigators presented at the 1st International Conference on Clinical and Scientific Advances in ME/CFS and Long COVID. Details regarding the agenda and event can be found on the event website. The two-day hybrid event was recorded. Both days of the conference are available below.
Day 1 (April 3, 2024): Dr. Susan Levine presented “Brief History of ‘Pandemics’ Related to ME/CFS Punta Gorda Florida and Royal Free Hospital in London. Origin of Current Case Definition.” Her talk starts at 27:00. Dr. Levine also took part in a panel discussion and “Conversation: The Role of Physician as Advocate, Lessons Learned from 30 Years of Clinical Practice” that occurred later in the day.
Day 2 (April 4, 2024): Dr. Maureen Hanson presented “Circulating Signals of ME/CFS.” Her talk starts at 6:07:00.
Op-ed aims to promote funding for ME/CFS
Maureen Hanson, Center Director, and journalist Hillary Johnson co-authored an op-ed in The Hill. The op-ed highlights the need to fund research into chronic post-infectious diseases. It is unfortunate that other similar, yet distinct, diseases such as ME/CFS are not included in long COVID funding proposed by Senator Sanders.. Please take a moment to read and share this op-ed to help promote funding for pre-pandemic ME/CFS–a disease that profoundly impacts so many people.
Dysregulation of EV protein cargo in ME/CFS females in response to maximal exercise
Exertion intolerance and post-exertional malaise are defining features of ME/CFS. Work from our Center aims to uncover the molecular disruption that occurs during and around these features. Thus, through the lens of extracellular vesicles (EVs), a publication from co-lead authors Ludovic Giloteaux and Katherine Glass provides novel insights into these topics.
The study involved the isolation of EVs, membrane-bound non-replicating particles released from cells, from the plasma of 18 ME/CFS and 17 healthy control female participants. The cargo of EVs are relevant in that they provide signals that could uncover elements of dysfunction in ME/CFS. Specifically, protein cargo from EVs were examined in this publication before and after a cardiopulmonary exercise test (i.e., around the induction of PEM).
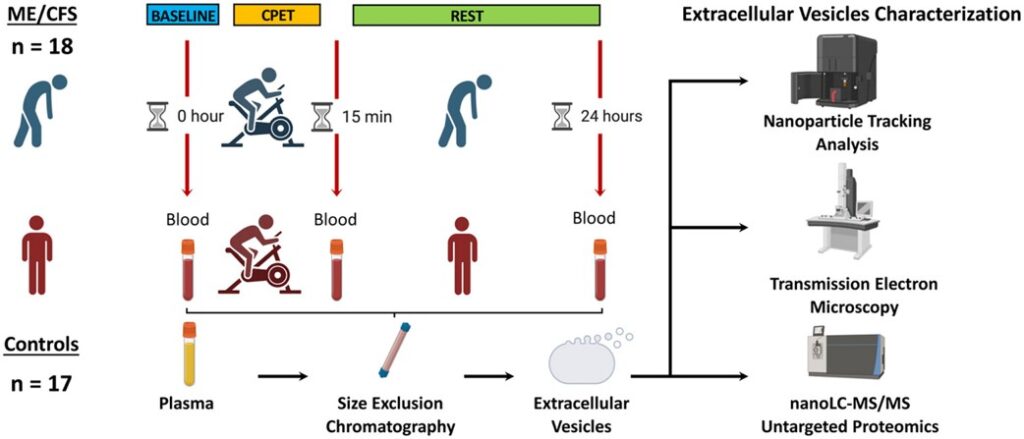
The EV proteome in response to exercise was clearly different in ME/CFS when compared to sedentary controls. These divergent responses were associated with different molecular pathways. Uncovered protein differences between the cohorts also point to contrasting tissues and cell types. Additionally, there were several proteins associated with a worsening of muscle pain (e.g., THBS1 and TPM4), PEM (e.g., NEXN), and fatigue (e.g., CLU) post exercise in ME/CFS. Although it is difficult to directly associate changes with the EV proteome to distinct cell types, this publication brings forth avenues to interrogate further.
If you are interested in more information regarding this publication, the entire paper is freely available in the Journal of Extracellular Vesicles.
Center participates in the NIH ME/CFS Research Roadmap series
The working group of the National Advisory Neurological Disorders and Stroke Council, part of the National Institutes of Health, recommended the development of research priorities for ME/CFS to help move the field towards translational research and clinical trials. The result led to creation of the ME/CFS Research Roadmap Working Group. The Group, co-led by Drs. Lucinda Bateman and Maureen Hanson, produced a series of eight webinars. A complete description of the webinar series can be found on the ME/CFS Research Roadmap website.
Our Center’s mission is to promote research to identify its cause(s), biomarkers, and pathophysiology in order to lead to prevention and effective treatments. With this focus, several Center investigators presented data to support the development of research priorities for ME/CFS. The talks from our Center are included below.
Maureen Hanson presented “ Immune cell-type approaches to identify mechanisms of ME/CFS” during the Immune System webinar. Her talk starts at 1:38:40.
Jessica Maya presented “Investigations and Consequences of Altered Metabolism in ME/CFS Immune Cells” during the Metabolism webinar. Her talk starts at 58:32.
Maureen Hanson presented “Chronic infection in ME/CFS: non-Herpes viruses” during the Chronic Infections webinar. Her talk starts at 1:01:25.
Ludovic Giloteaux presented “Extracellular vesicles” during the Physiology webinar. His talk starts at 3:15:10.
The NIH ME/CFS Center presents lectures at “Advancing ME/CFS Research: Identifying Targets for Intervention and Learning from Long COVID”

NIH held a hybrid online conference on the NIH campus on December 11-12, 2023. Center personnel attending in person were Claire McNally, Annie Gardella, David Iu, Jessica Maya, Tien Luyen (“Louis”) Vu, Katherine Glass, Arnaud Germain, Ludovic Giloteaux, Dawei Li, Andrew Grimson, and Maureen Hanson, as well as collaborator Nicholas Hampilos from Weill Cornell Medicine.
Both days of the conference are available online.
Jessica Maya’s presentation “Investigating T cell populations for immune cell dysfunction in ME/CFS” starts at 3:50:10.
Maureen Hanson’s presentation on “ME/CFS and long COVID: similarities and differences” starts at 1:03:00.
Andrew Grimson’s presentation on “Monocyte dysregulation in ME/CFS” starts at 1:37:35.
Nicholas Hampilos’ presentation on “Effect of Physical Exertion on CNS Oxidative Stress and Metabolism in ME/CFS” starts at 2:56:53.
Center trainees participate in the Symposium For Promoting The Advancement Of Research Knowledge In ME/CFS (SPARK ME)

NIH sponsored an early career researchers workshop on December 10, 2023 attended by Cornell graduate students Claire McNally Annie Gardella, and David Iu, postdoctoral associates Jessica Maya and Tien Luyen (“Louis”) Vu, and Research Associates Katherine Glass, Arnaud Germain and Ludovic Giloteaux. Drs. Glass and Maya helped organize the meeting.
Verbal presentations:
David Iu: Epigenetic Reprogramming of CD8+ T cell Populations Drives Exhaustion in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)
Tien Luyen Vu: Single-cell transcriptomics of ME/CFS circulating immune system before and after symptom provocation
Poster presentations:
Anne Gardella: Cell-free RNA signatures of myalgic encephalomyelitis/ chronic fatigue syndrome
Ludovic Giloteaux: Extracellular vesicle protein cargo in ME/CFS cases and controls following maximal exercise
Arnaud Germain: Proteomic adjustments following induction of post-exertional malaise
Claire McNally: Investigating the role of iNOS in endothelial dysfunction in ME/CFS
ME/CFS lecture presented at the Viral Infections and Inflammation Workshop in Rockville, Maryland September 6-7, 2023
In an NIH-sponsored workshop featuring studies of long COVID, acute COVID19, HIV/AIDS, viral encephalitis, Epstein-Barr Virus, Ebola virus, Endogenous retroviruses, Maureen Hanson presented a talk entitled “Viruses, Immune Dysfunction, and ME/CFS”
All talks can be accessed through the following website after free registration here or on the Academic Medical Education’s YouTube channel. Maureen Hanson’s talk is included below.
 Center for Enervating NeuroImmune Disease
Center for Enervating NeuroImmune Disease




